Music, movies and television are getting louder but, sadly, many people aren’t noticing. If you find yourself turning the volume up instead of down, you may be one of the millions suffering sensorineural hearing loss.
Sensorineural hearing loss affects most people gradually, increasing with age or prolonged exposure to excessive noise. It is rarely correctable by surgery and until now, hearing aids were the only solution.
A Better Alternative


Carlos Rodriguez has run his barbershop in the Pacific Mutual Building for 30 years. (Photo/Your Credit Here)
New technology may soon change that picture for those with moderate to severe sensorineural hearing loss. Dr. Jack Shohet, director of neurotology for UCI Medical Center, is one of a handful of surgeons throughout the U.S. now able to implant a new middle ear hearing device.
“UCI Medical Center is among the first in the nation—and the only Orange County-based medical center-to offer this procedure,” says Shohet. “It’s an exciting time to be in this field of medicine. Some highly remarkable alternatives to the standard hearing aid are emerging.” The Soundbridge™ implant is one of these remarkable new alternatives.
Developed by Symphonix Devices Inc., and recently approved by the Food and Drug Administration, this device goes far beyond the science of traditional hearing aids, which merely amplify sound.
“Some highly remarkable alternatives to the standard hearing aid are emerging.”
Simulating Natural Hearing

Carlos Rodriguez has run his barbershop in the Pacific Mutual Building for 30 years. (Photo/Your Credit Here)
The implant uses a processor to transmit sound and directly vibrate the middle ear bones, simulating natural hearing. It delivers greater fidelity while virtually eliminating feedback-that high-pitched whistle often associated with hearing aids. It may even benefit patients who can’t otherwise wear a hearing aid in their ear canal.
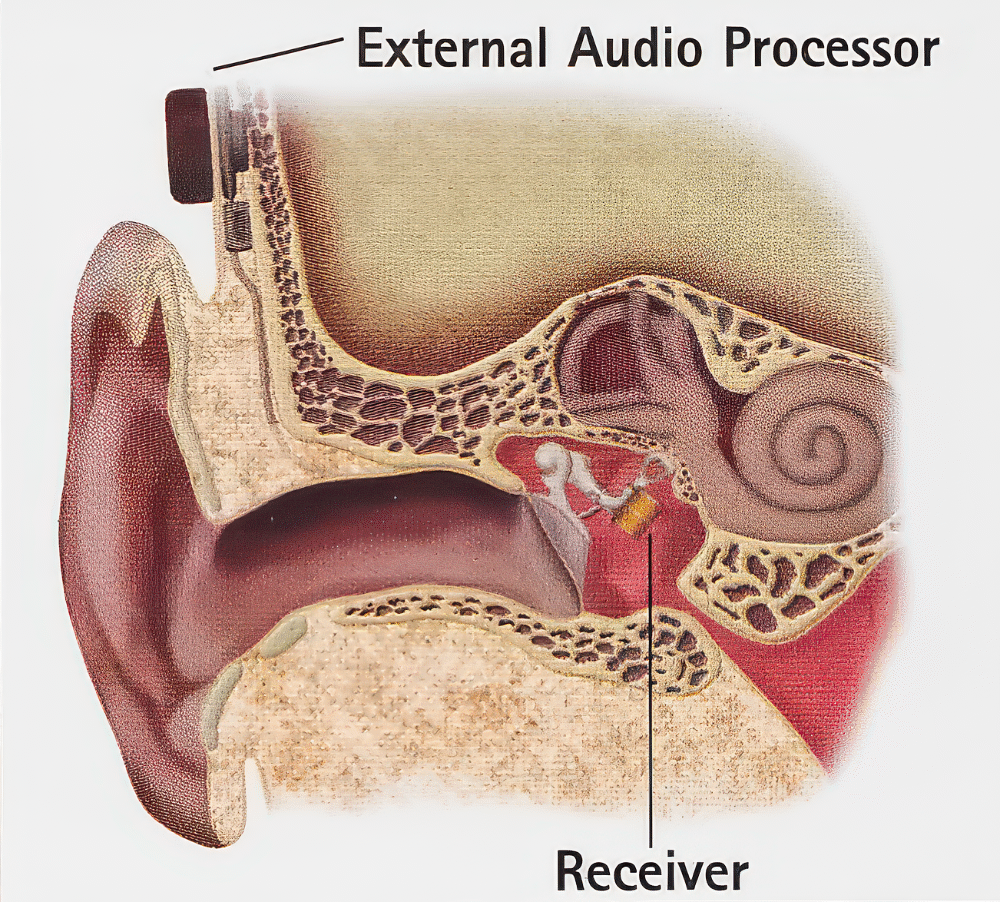
The device consists of two units: the receiver, implanted internally, and an external audio processor, attached magnetically behind the ear, where it can be hidden by the hairline.
“Patients can go home a few hours after surgery,” explains Shohet. “Four to six weeks later, after they’re fully healed, they return to their audiologist to activate the device, which is fine-tuned for each individual.”
As simple as the procedure may appear, however, it’s not for everyone. Candidates must undergo extensive evaluation to determine eligibility for surgery. Moreover, the device is not recommended for persons with conductive hearing loss or certain other types of auditory disorder.
A Big Step Forward
“This is a tremendous leap forward for people who have been waiting a long time in frustration,” says Shohet. “No doubt, with time, technology like this will become increasingly accessible to more and more patients” To schedule an appointment with Dr. Shohet, and see if you are a candidate for this surgery, call toll free1-877-UCI-DOCS or visit us online at www.ucihealth.com.
Touching Life’s Blueprint
Genetics is one of the most fascinating areas of medicine. For the general public, however, the word often evokes misconceptions bordering on science fiction. In reality, genetics touches the lives of young and old at basic levels every day.
The work of Dr. Suzanne Cassidy, chief of UCI Medical Center’s division of human genetics, is a case in point. Cassidy specializes in the full spectrum of genetic diagnosis and counseling, but takes special interest in mental retardation in children. Her expertise offers welcome guidance to families and children affected by mental retardation, which appears in approximately three to five percent of the population.
Following the Genetic Trail


Carlos Rodriguez has run his barbershop in the Pacific Mutual Building for 30 years. (Photo/Your Credit Here)
The genes found on our chromosomes and their arrangement determine our individual characteristics. Disruptions of genes or their expression can result in illness or abnormality. Of the thousands of known genetic disorders, more than 100 can lead to mental retardation. Diagnosis of specific causes is based on a variety of evaluations, including a patient’s appearance, family history and genetic tests (normally performed on white blood cells).
“We can accurately determine the genetic causes in more than half of our patients,” says Cassidy. “This helps us recommend the best medical treatment and schooling to optimize the individual’s potential. We can also assess family risk factors for couples before they have children”
Respecting Patients
Inevitably, the subject of genetics raises ethical concerns, especially when it touches on the family. Cassidy is sensitive to this. “Privacy of genetic information is a big issue,” she says. “People fear discrimination. We take great pains to ensure confidentiality. Also, we respect people’s backgrounds and beliefs in making decisions.”
Taking it One Day at a Time
While breakthrough discoveries and miracle cures may capture public imagination, the real work of geneticists boils down to improving the day-to-day lives of patients and families.
“We can accurately determine the genetic causes [of mental retardation] in more than half of our patients.”
“Medicine is not yet able to fix the genetic factors that lead to mental retardation,” explains Cassidy. “However, we have tremendous tools to help families make sound treatment decisions and increase the happiness and health of their children.” For more information or a referral to UCI Medical Center’s genetics program, call toll free 1-877-UCI-DOCS.
Medicine With Muscle
Linda couldn’t understand it. Over the course of a few weeks it became more difficult to climb stairs and comb her hair. No numbness-just a mild ache in her muscles and a sense of weakness. With time the problem only worsened, and ultimately included difficulty in swallowing and breathing. She called her physician, who referred her to a specialist.
The diagnosis came as a shock: polymyositis, a rare neuromuscular disorder that most commonly afflicts women under the age of 40. Suddenly the questions flooded in: Is it fatal? Can it be treated? What future can I expect?
Finding the Right Answers


Carlos Rodriguez has run his barbershop in the Pacific Mutual Building for 30 years. (Photo/Your Credit Here)
Answering questions like Linda’s is a specialty for Dr. Tahseen Mozaffar, director of UCI Medical Center’s neuromuscular program. His expertise includes inherited and acquired disorders of the nerves, muscles, spinal cord, and neuromuscular junction— including myasthenia gravis, ALS (or Lou Gehrig’s disease), and Duchenne muscular dystrophy.
“Some patients go from physician to physician in search of answers when time is of the essence.”
According to Mozaffar, neuromuscular diseases can run different courses in different patients, sometimes at a fast pace, making quick, certain diagnoses essential. Fortunately, today’s technology can do more than merely identify such disorders-it can project how they will play out in each person.
“In addition to electromyography (EMG), our chief tool is nerve and muscle pathology,” explains Mozaffar. “We can analyze muscle and nerve samples with great accuracy and predict other problems that may appear in the patient, as well as the complications they will experience. This helps us implement aggressive treatments ahead of time”
Improving the Quality of Life
While polymyositis is not always fatal, other disorders like ALS or Duchenne typically are. As they progress, muscles throughout the body weaken and lose function. Respiratory failure is a frequent concern. With no known cures, treatment focuses on slowing the progress of these diseases to help patients remain active for longer, more fulfilling lives.
“These disorders can be difficult to identify,” says Mozaffar. “Some patients go from physician to physician in search of answers when time is of the essence Our procedures allow us to make a firm diagnosis in 10-15 days, sometimes less.”
Taking a Leading Role
Mozaffar sees UCI Medical Center playing a leading role in developing better treatments-and eventual cures “UCI-based researchers are engaged in groundbreaking neuromuscular research. Even if there aren’t a lot of answers now, there will be. And this will be the place to find them.”